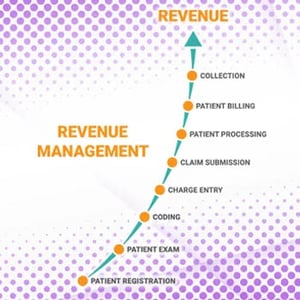
As a result of the pandemic U.S. healthcare faces staggering revenue losses.
"The pandemic could cause U.S. hospitals to face between $53 billion and $122 billion in revenue loss this year, according to a study from healthcare consulting firm Kaufman Hall commissioned by the American Hospital Association." Source: Becker Hospital Review
This decline puts tremendous pressure on medical revenue cycle management (RCM).
 Add to that the fact that many health systems are adopting value-based payment models and becoming Accountable Care Organizations. It’s clear that management of information is more important today than ever before.
Add to that the fact that many health systems are adopting value-based payment models and becoming Accountable Care Organizations. It’s clear that management of information is more important today than ever before.
The key to rapidly achieving sustained net operating margin is optimizing the revenue cycle through better information management.
The Missing Piece of Tech to Optimize Your Medical Revenue Cycle Management
Top performing hospital systems are using data tools to spend less money on critical tasks like:
- Data input
- Healthcare claims processing
- Supply chain logistics
But the proliferation of new "artificially intelligent" software solutions with vendors more focused on hype than results has muddied the technology waters.
 What's needed today is intelligent connectivity between core hospital systems - solutions that empower data strategy and optimize the
What's needed today is intelligent connectivity between core hospital systems - solutions that empower data strategy and optimize the
revenue cycle. Lean revenue cycle management is a methodology that ensures each step in the process is valuable, optimized, and maximizes resources.
For many healthcare organizations, intelligent connectivity between
upstream and downstream software applications is the crucial missing piece. Today’s advanced artificial intelligence software brings a new level of connectivity and interoperability.
7 Examples of Tech Powering Medical Revenue Cycle Management
This article discusses several ways that tech such as machine learning or natural language processing - and logic-based solutions like robotic process automation / intelligent document processing - are being used to increase net revenue:
- Insurance Verification / Eligibility
- Data Entry - Patient Demographics
- Medical Records / Billing
- Claims Processing
- Retrospective Denial Management
- Managed Care Contracts
- Supply Chain
1. Insurance Verification / Eligibility
Manual insurance coverage verification is error-prone and costly. Healthcare centers that don’t collect deductibles upfront, or collect the wrong amount, suffer huge revenue losses. This is an especially critical situation as more patients have higher deductibles and maximums.
 Lean medical revenue cycle management dictates that more time should be spent on eligibility and claim acceptance before claims are ever submitted.
Lean medical revenue cycle management dictates that more time should be spent on eligibility and claim acceptance before claims are ever submitted.
Automating insurance verification and eligibility workflows ensures more time is spent getting claims right the first time.
2. Initial Data Entry - Patient Demographics
Accurate data entry of patient demographic information is critical for claims processing. Strive to create workflows that validate information and flag any record missing documentation in order to have accurate data and minimize manual entry.
Intelligent software platforms can help with this, as they read forms and recognizes checkboxes without requiring complex templates or human review. They streamline any paper, digital, or mixed content registration processes.
3. Medical Records / Billing
 Medical revenue cycle management systems can also be improved by eliminating manual data entry through intelligently processing electronic and paper explanation of benefit forms (EOBs).
Medical revenue cycle management systems can also be improved by eliminating manual data entry through intelligently processing electronic and paper explanation of benefit forms (EOBs).
They extract patient data from EOBs and migrate it to billing applications or electronic files for posting. As a result, you can easily achieve accurate integration of day-forward records with validation and patient look-ups.
Top RCM Benefits of Intelligent Data Processing:
- Automate EOB data capture
- Integrate with medical billing applications
- Decrease days in AR - recognize revenue quicker
- Index scanned and electronic documentation for quick retrieval
- Automate data extraction from lab and diagnostic results from any source
4. Claims Processing
Another way that modern tech is boosting lean medical revenue cycle management is by automating data entry / extraction on all standard claim forms and attachments.
High accuracy is achievable with solutions using validation rules to ensure billing, accounting, and practice management applications receive the most accurate data with very little manual effort.
Top Benefits of Claims Processing for Medical Revenue Cycle Management:
- Validate ICD and CPT codes
- Intelligently process any type of claim form, including CMS-1500 and UB-04/1450 without separator sheets
- CCLF file interface for integration, data matching, and reporting
- EDI data exports
- Focus on accurate submissions, not on denial management
5. Retrospective Denial Management
Retrospective denials are an industry silent killer of net revenue and leave providers vulnerable if they don’t act on a timely basis.
 These types of insurance denials or “take backs” do not pass through routine electronic channels (835), reversing revenue from paid claims for discharges that may have taken place months or years prior.
These types of insurance denials or “take backs” do not pass through routine electronic channels (835), reversing revenue from paid claims for discharges that may have taken place months or years prior.
Detecting these letters and notices and acting upon them is mission-critical for safeguarding net revenue.
An audit at one health system uncovered $12 million in annual take backs from retrospective reviews. The only way to manage take backs is to capture and route time-dependent correspondence to office staff for immediate and intensive follow-up.
In the case cited, losses were incurred due to the timeliness of follow-up with internal operations. Many providers experience this time and time again.
Using a retrospective denial platform empowers providers against retrospective take backs by quantifying risk and enabling timely action. It boosts efficiency by:
- Reducing time to process
- Eliminating significant lost revenue
- Progressively building intelligence by payor to help the provider continuously adjust workflows in response to payor changes in payment practices
6. Managed Care Contracting
 Ensure that managed care contracts are profitable and not causing a disproportionate share of administrative overhead. Intelligent software can increase the efficiency of revenue cycle management software by easily analyzing contracts for appropriate and reasonable language regarding Payors, Products, Covered Services, Claims, Prior Authorizations, Eligibility, Audits, Renewal Dates, etc.
Ensure that managed care contracts are profitable and not causing a disproportionate share of administrative overhead. Intelligent software can increase the efficiency of revenue cycle management software by easily analyzing contracts for appropriate and reasonable language regarding Payors, Products, Covered Services, Claims, Prior Authorizations, Eligibility, Audits, Renewal Dates, etc.
Support realistic cash flow projections based on cost calculations by
utilization and staff work time.
A Managed Care Contracting Advantages:
- Insight to drive negotiation on fee-for-service and capitated contracts
- Report on expenditures for operations and clinical services
- Integration with GL and accounting applications
- Support historical cost tracking
- Enhance billing and AR workflows
- Supplement utilization review processes
7. Supply Chain Logistics
Top performing hospitals have reduced supply chain costs by 17.8% – up to $9M per year – by leveraging evidence-based protocols and data analytics. These methods of medical revenue cycle management reduce pricing variances and product use while increasing positive clinical outcomes.
Streamline supply chain workflows and ensure accuracy by performing automated validations on vendor and utilization data.
Top Benefits of Revenue Cycle Management Software:
- Capture and extract near real-time data from paper and digital sources
- Validations and workflow for the entire procurement process; from requisition to final EDI / upload
- Procurement application integrations
- Provide data for activity-based budgeting initiatives
- Supplier contract and pricing validation
- Data processing for Procure-to-Pay initiatives
This article was last updated 4/29/2021.
About the Author: Brad Blood
Senior Marketing Specialist at BIS